This content is also available in:
Italiano
Português
Deutsch
The epithelium that lines the endocervical canal and endocervical crypts consists of a single layer of mucus-producing columnar cells. These cells are tall and cylindrical and are arranged in a picket fence formation. The nuclei are mostly situated basally, adjacent to the basement membrane, but during active mucous secretion the nucleus can be displaced by the mucus and pushed towards the centre.
In inflammation, there may be mucus depletion in which the endocervical cells are less tall and mitoses (or MIB-1 positivity) may occasionally be seen in the absence of neoplasia or pre-neoplasia.
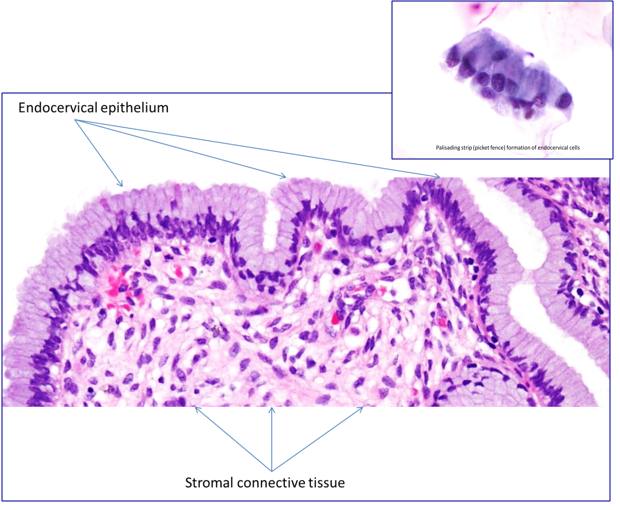
The secretory endocervical cells begin at the squamocolumnar junction and line the endocervix and the endocervical crypts; they are mucus-producing cells that form a mucus plug to prevent bacterial and fungal infection of the uterus.
The ciliated cells are most numerous at the endometrial/endocervical junction. Their main function is to actively carry the mucus along the mucous membrane. They may be seen elsewhere in the endocervix as tubal metaplasia or tubo-endometrioid metaplasia, usually after instrumentation such as cone biopsy.
The reserve cells are small cuboidal cells lying deep to the columnar cells, which are more prominent during the metaplastic process and are the cells from which it arises. Reserve cells are predominantly found in the transformation zone and can be identified by a different immunoprofile compared with overlying columnar cells
Endocervical crypts extend to between 0.5 and 1.0 cm in depth below the epithelial surface.

